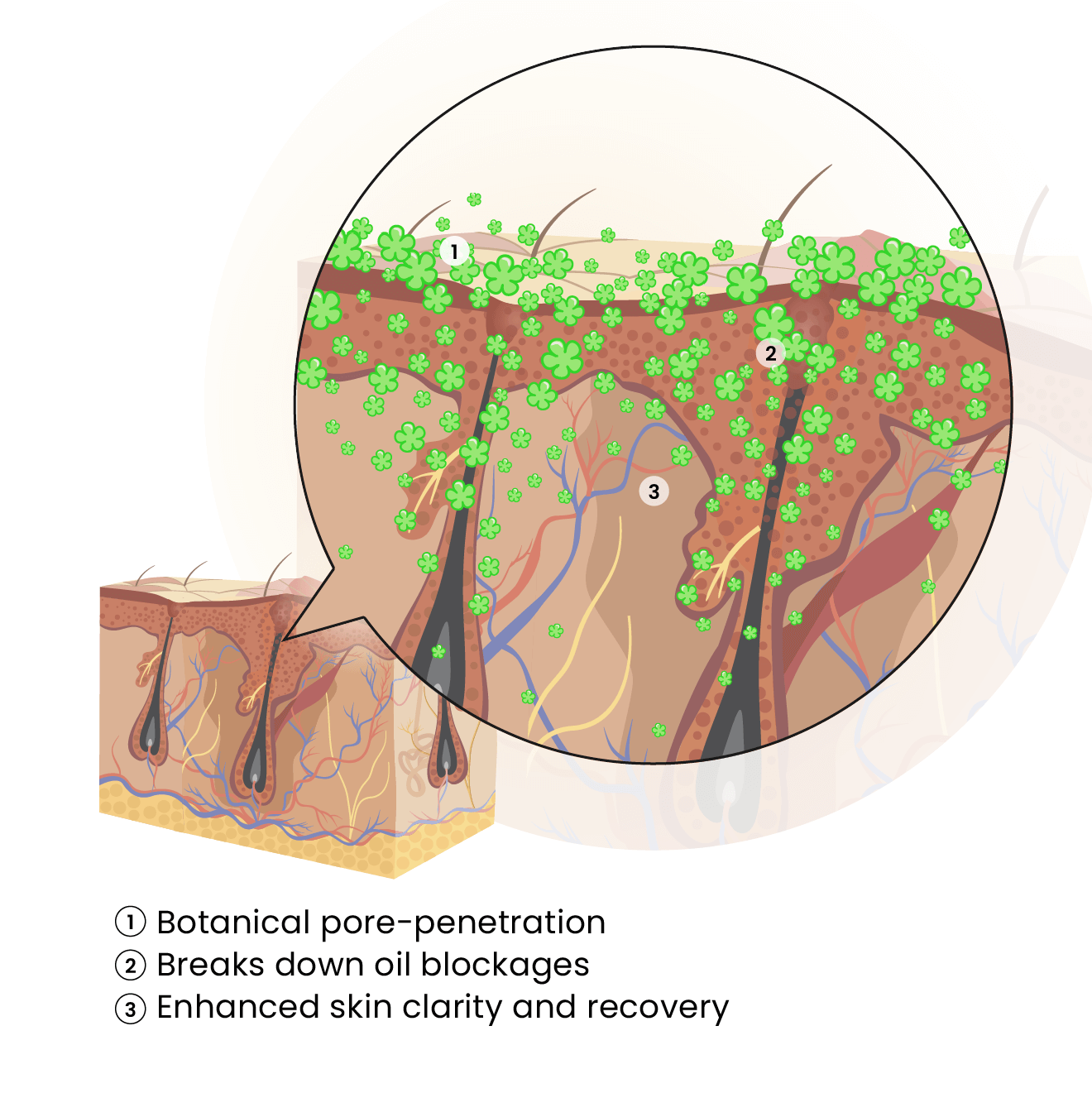
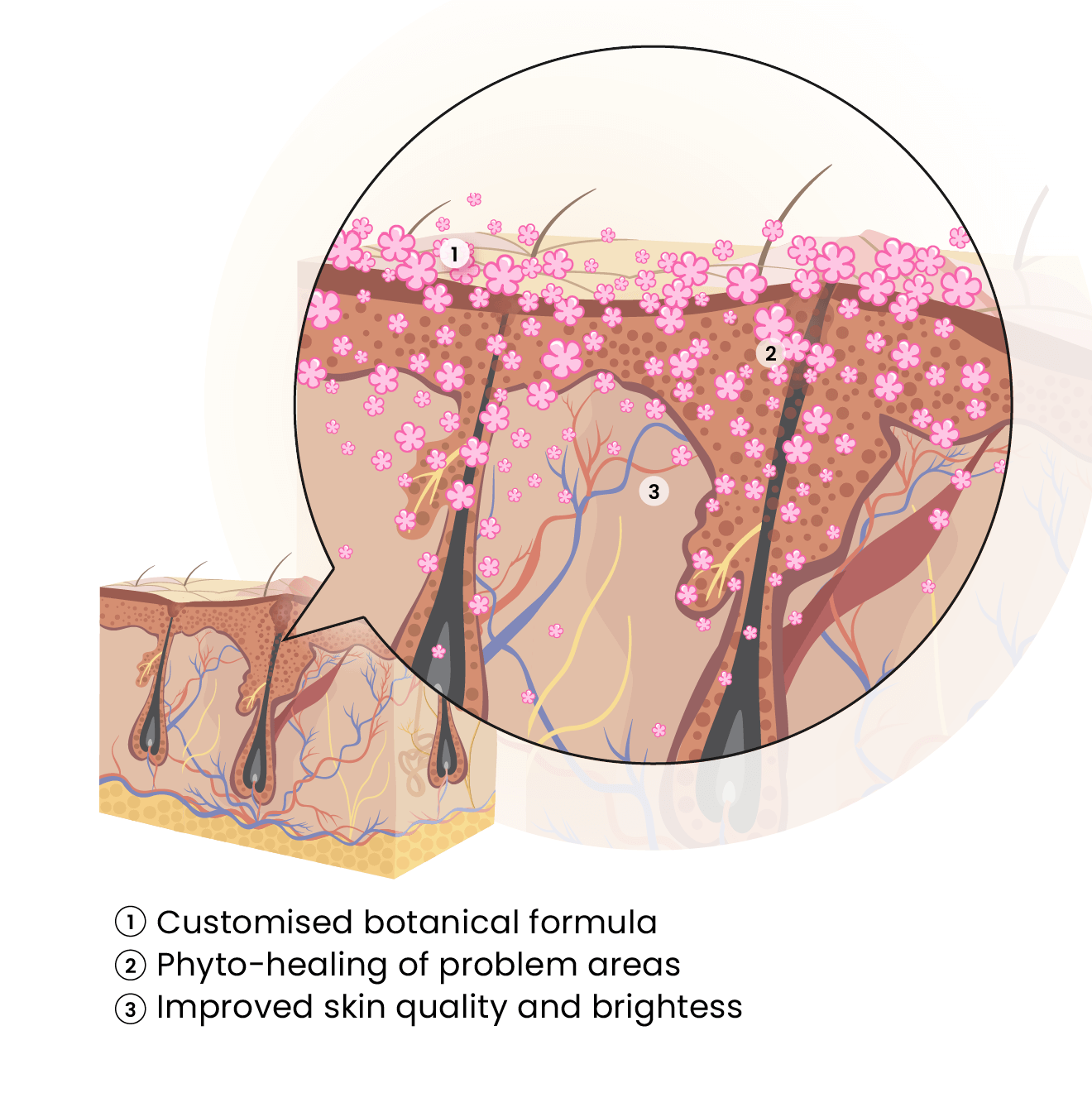
What is PhytoClear
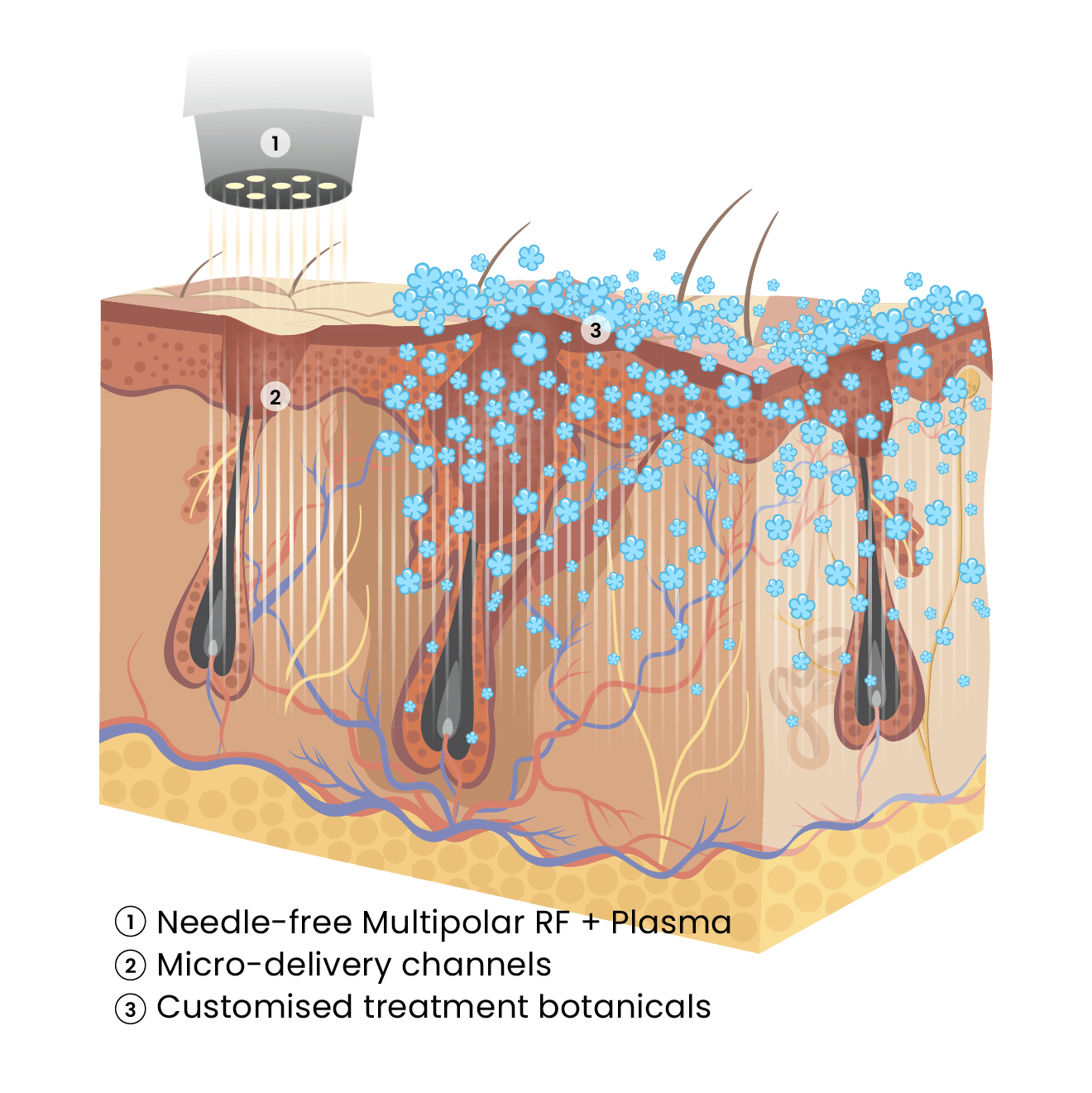
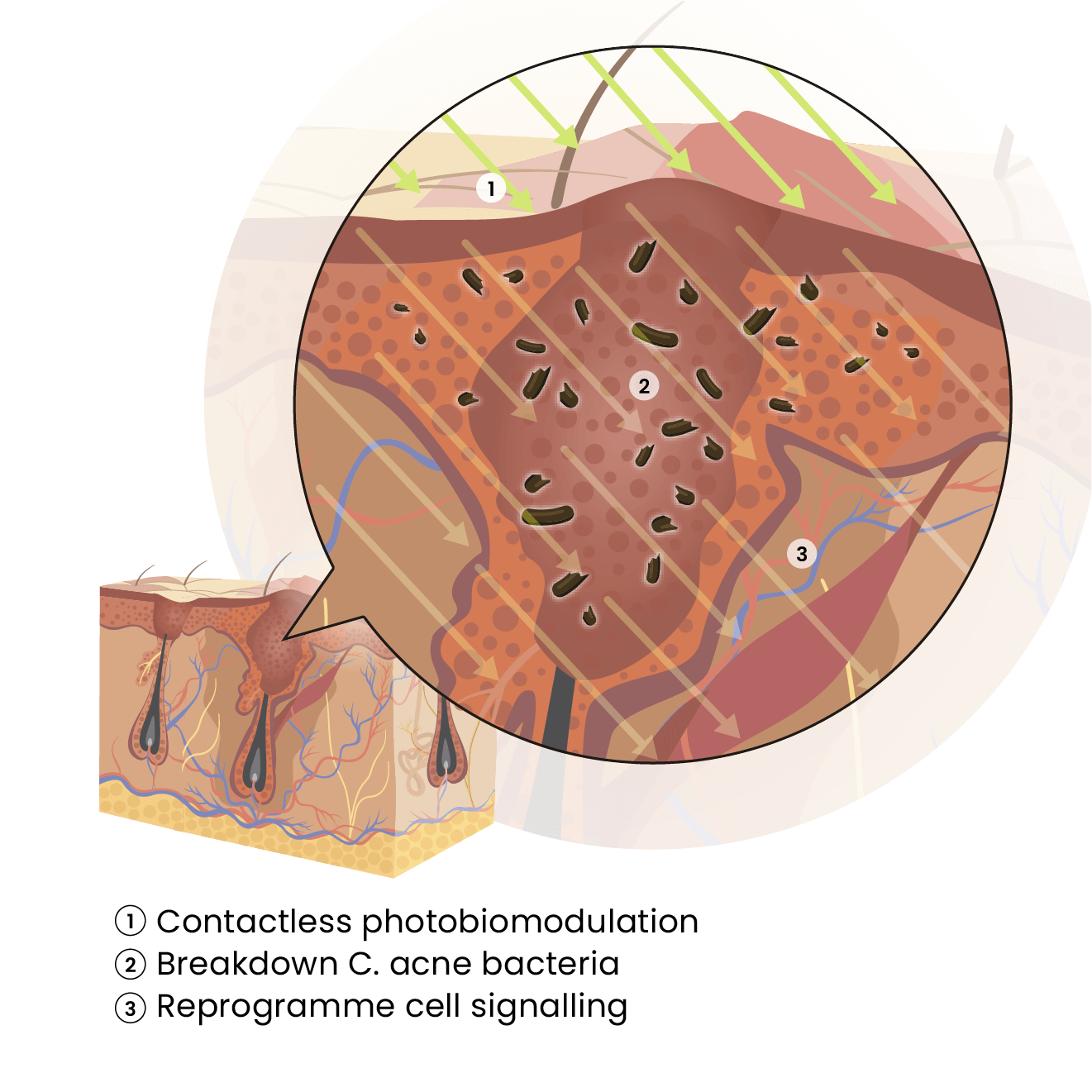
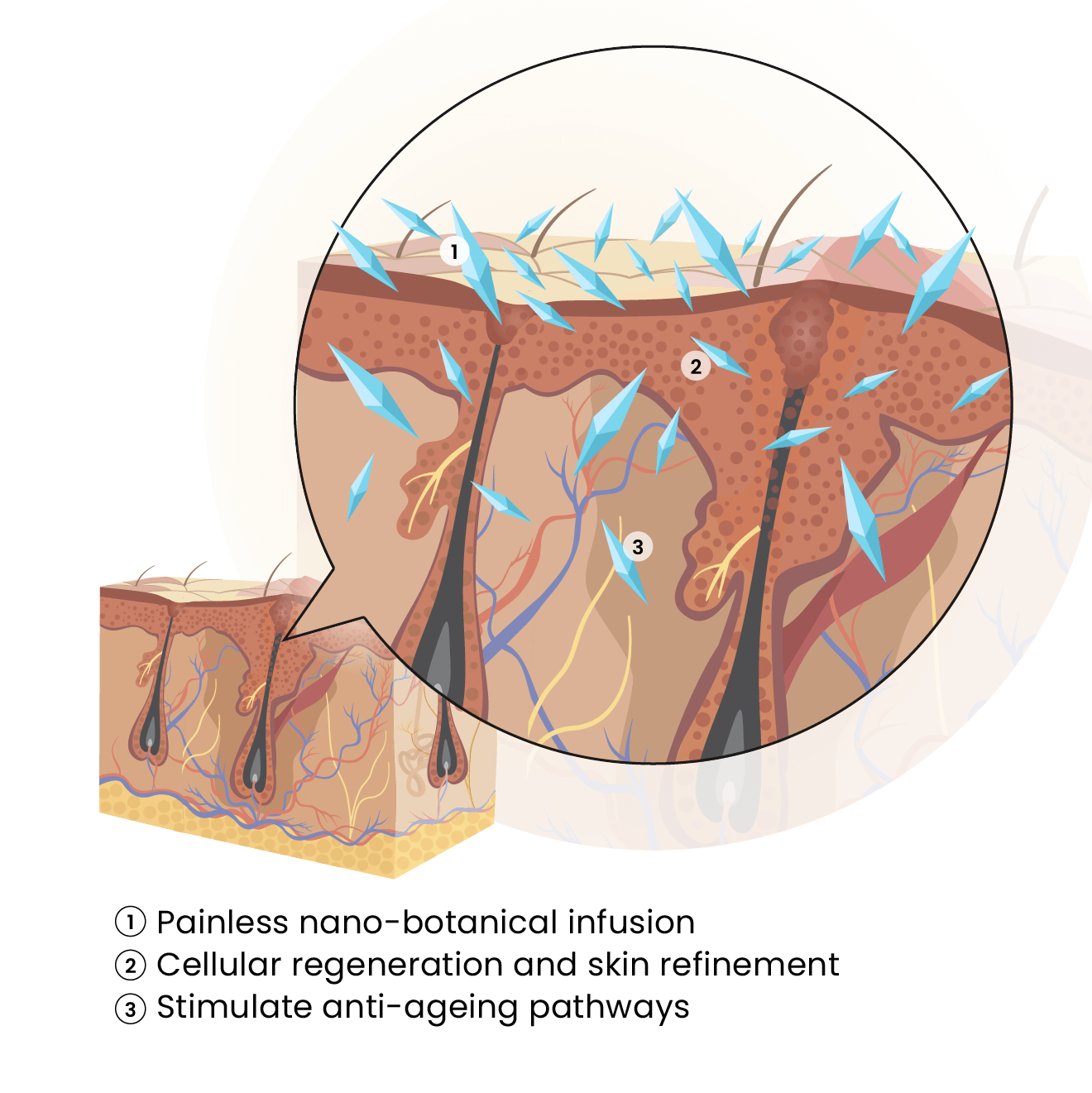
How It Works
Who Is It For
How Is It Different
| Mainstream Methods | PhytoClear™ Approach |
|---|---|
| Antibiotics, medication, harsh topicals | Gentle, skin-compatible botanicals and marine actives |
| Quick fixes that overlook root causes | Targets inflammation, bacteria, and oil imbalance |
| Surface-only relief with frequent relapse | Builds internal balance and lasting skin resilience |
| Side effects like peeling or rebound | Friendlier for sensitive and hormonal skin |
| Barrier damage and scarring risk | Strengthens barrier and reduces post-acne marks |
| One-size-fits-all treatments | Personalised to your skin’s needs and triggers |
Begin Your Clear Skin Reset ✧
Thiboutot D et al., “New insights into the management of acne: An update from the Global Alliance to Improve Outcomes in Acne Group.” Journal of the American Academy of Dermatology 60, no. 5 (2009): S1-S50.
Tanghetti EA, “The role of inflammation in the pathology of acne.” Journal of Clinical and Aesthetic Dermatology 6, no. 9 (2013): 27-35.
Sivamani RK et al., “Natural alternatives for treating acne and skin inflammation.” Journal of Drugs in Dermatology 18, no. 8 (2019): 788-794.
Fabbrocini G et al., “The role of sebum and sebaceous glands in acne pathogenesis.” Journal of the American Academy of Dermatology 66, no. 6 (2012): 939-949.
Grice EA et al., “The skin microbiome and its role in acne.” Nature Reviews Microbiology 9, no. 4 (2011): 244-253.
Bowe WP et al., “The effects of diet on acne: A review of the evidence.” Journal of the American Academy of Dermatology 63, no. 1 (2010): 124-141.
Kraft JN et al., “The role of inflammation in acne management.” Journal of Clinical and Aesthetic Dermatology 11, no. 8 (2018): 16-23.
Cunliffe WJ et al., “Pathogenesis of acne.” British Journal of Dermatology 139, no. 5 (1998): 1-5.
Bikowski JB et al., “Prevention and management of post-inflammatory hyperpigmentation in acne.” Journal of Drugs in Dermatology 17, no. 9 (2018): 925-932.
Passeron T et al., “Post-inflammatory hyperpigmentation in acne: Pathogenesis and treatments.” Dermatologic Clinics 32, no. 3 (2014): 291-299.
Rodriguez CI et al., “Role of oxidative stress in acne and its management.” Journal of Clinical and Aesthetic Dermatology 12, no. 4 (2019): 28-35.
Verallo-Rowell VM et al., “Safety and efficacy of botanical agents in acne management.” Dermatologic Therapy 33, no. 5 (2020): e13963.
Alvarez OM et al., “Botanical extracts for treating acne: Efficacy and safety.” Journal of Cosmetic Dermatology 17, no. 6 (2018): 1067-1074.
Draelos ZD et al., “Efficacy of natural ingredients in anti-acne treatments.” Journal of Drugs in Dermatology 18, no. 6 (2019): 586-591.
Del Rosario C et al., “Tyrosinase inhibitors: Strategies to control melanin production in acne-induced hyperpigmentation.” International Journal of Molecular Sciences 22, no. 11 (2021): 6150.
Sardana K et al., “Rebound acne and its management: A review.” Indian Journal of Dermatology, Venereology, and Leprology 85, no. 3 (2019): 243-250.
Narins RS et al., “Long-term complications of injectable soft tissue fillers in acne scars.” Dermatologic Surgery 34, no. 12 (2008): 1574-1579.
Boonchai W et al., “Post-inflammatory hyperpigmentation: Risk factors and prevention.” International Journal of Dermatology 55, no. 5 (2016): 487-495.
Grimes PE et al., “Histologic changes in acne-prone skin.” Journal of the American Academy of Dermatology 55, no. 5 (2006): 768-775.
Lim JT et al., “Sun protection and prevention of post-inflammatory hyperpigmentation in acne.” Journal of the American Academy of Dermatology 82, no. 5 (2020): 1236-1245.
Sadick NS et al., “The impact of collagen production on acne scars.” Journal of Clinical and Aesthetic Dermatology 13, no. 6 (2020): 18-25.
Handog EB et al., “Challenges in the management of acne: Prevention and treatment.” Journal of Clinical and Aesthetic Dermatology 9, no. 1 (2016): 15-24.
Hassim Z et al., “Management of collagen depletion and fat layer loss in acne-prone skin.” Journal of Dermatology 47, no. 5 (2020): 431-437.
Grice EA et al., “The skin microbiome and acne pathophysiology.” Nature Reviews Microbiology 9, no. 4 (2011): 244-253.
Nistico SP et al., “Efficacy of botanical formulations for managing acne and hyperpigmentation.” Journal of Dermatological Treatment 31, no. 4 (2020): 395-402.
Thiboutot D et al., “New insights into the management of acne: An update from the Global Alliance to Improve Outcomes in Acne Group.” Journal of the American Academy of Dermatology 60, no. 5 (2009): S1-S50.
Tanghetti EA, “The role of inflammation in the pathology of acne.” Journal of Clinical and Aesthetic Dermatology 6, no. 9 (2013): 27-35.
Sivamani RK et al., “Natural alternatives for treating acne and skin inflammation.” Journal of Drugs in Dermatology 18, no. 8 (2019): 788-794.
Grimes PE et al., “Histologic changes in acne-prone skin.” Journal of the American Academy of Dermatology 55, no. 5 (2006): 768-775.
Draelos ZD et al., “Efficacy of natural ingredients in anti-acne treatments.” Journal of Drugs in Dermatology 18, no. 6 (2019): 586-591.
Bowe WP et al., “The effects of diet on acne: A review of the evidence.” Journal of the American Academy of Dermatology 63, no. 1 (2010): 124-141.
Del Rosario C et al., “Tyrosinase inhibitors: Strategies to control melanin production in acne-induced hyperpigmentation.” International Journal of Molecular Sciences 22, no. 11 (2021): 6150.
Fabbrocini G et al., “The role of sebum and sebaceous glands in acne pathogenesis.” Journal of the American Academy of Dermatology 66, no. 6 (2012): 939-949.
Grice EA et al., “The skin microbiome and its role in acne.” Nature Reviews Microbiology 9, no. 4 (2011): 244-253.
Kraft JN et al., “The role of inflammation in acne management.” Journal of Clinical and Aesthetic Dermatology 11, no. 8 (2018): 16-23.
Cunliffe WJ et al., “Pathogenesis of acne.” British Journal of Dermatology 139, no. 5 (1998): 1-5.
Boonchai W et al., “Post-inflammatory hyperpigmentation: Risk factors and prevention.” International Journal of Dermatology 55, no. 5 (2016): 487-495.
Rodriguez CI et al., “Role of oxidative stress in acne and its management.” Journal of Clinical and Aesthetic Dermatology 12, no. 4 (2019): 28-35.
Alvarez OM et al., “Botanical extracts for treating acne: Efficacy and safety.” Journal of Cosmetic Dermatology 17, no. 6 (2018): 1067-1074.
Passeron T et al., “Post-inflammatory hyperpigmentation in acne: Pathogenesis and treatments.” Dermatologic Clinics 32, no. 3 (2014): 291-299.
Verallo-Rowell VM et al., “Safety and efficacy of botanical agents in acne management.” Dermatologic Therapy 33, no. 5 (2020): e13963.
Poon TS et al., “Age-related changes in acne and effective management strategies.” Journal of Clinical and Aesthetic Dermatology 14, no. 7 (2021): 32-40.
Handog EB et al., “Challenges in the management of acne: Prevention and treatment.” Journal of Clinical and Aesthetic Dermatology 9, no. 1 (2016): 15-24.
Bikowski JB et al., “Prevention and management of post-inflammatory hyperpigmentation in acne.” Journal of Drugs in Dermatology 17, no. 9 (2018): 925-932.
Hassim Z et al., “Management of collagen depletion and fat layer loss in acne-prone skin.” Journal of Dermatology 47, no. 5 (2020): 431-437.
Grimes PE et al., “Management of exogenous ochronosis caused by topical hydroquinone in acne-prone skin.” Journal of Dermatology 47, no. 5 (2020): 431-437.
Narins RS et al., “Long-term complications of injectable soft tissue fillers in acne scars.” Dermatologic Surgery 34, no. 12 (2008): 1574-1579.
Lim JT et al., “Sun protection and prevention of post-inflammatory hyperpigmentation in acne.” Journal of the American Academy of Dermatology 82, no. 5 (2020): 1236-1245.
Sardana K et al., “Rebound acne and its management: A review.” Indian Journal of Dermatology, Venereology, and Leprology 85, no. 3 (2019): 243-250.
Grice EA et al., “The skin microbiome and acne pathophysiology.” Nature Reviews Microbiology 9, no. 4 (2011): 244-253.
Del Rosso JQ et al., “Antibiotic resistance: A comprehensive review of management strategies for acne.” Journal of Clinical and Aesthetic Dermatology 13, no. 9 (2020): 22-28.
Leyden JJ et al., “Antibiotic resistance in acne treatment: A review of the implications.” Journal of the American Academy of Dermatology 68, no. 2 (2013): 295-305.
Thiboutot D et al., “New insights into the management of acne: An update from the Global Alliance to Improve Outcomes in Acne Group.” Journal of the American Academy of Dermatology 60, no. 5 (2009): S1-S50.
Tanghetti EA, “The role of inflammation in the pathology of acne.” Journal of Clinical and Aesthetic Dermatology 6, no. 9 (2013): 27-35.
Sivamani RK et al., “Natural alternatives for treating acne and skin inflammation.” Journal of Drugs in Dermatology 18, no. 8 (2019): 788-794.
Grice EA et al., “The skin microbiome and its role in acne.” Nature Reviews Microbiology 9, no. 4 (2011): 244-253.
Bowe WP et al., “The effects of diet on acne: A review of the evidence.” Journal of the American Academy of Dermatology 63, no. 1 (2010): 124-141.
Fabbrocini G et al., “The role of sebum and sebaceous glands in acne pathogenesis.” Journal of the American Academy of Dermatology 66, no. 6 (2012): 939-949.
Rodriguez CI et al., “Role of oxidative stress in acne and its management.” Journal of Clinical and Aesthetic Dermatology 12, no. 4 (2019): 28-35.
Del Rosario C et al., “Tyrosinase inhibitors: Strategies to control melanin production in acne-induced hyperpigmentation.” International Journal of Molecular Sciences 22, no. 11 (2021): 6150.
Grimes PE et al., “Histologic changes in acne-prone skin.” Journal of the American Academy of Dermatology 55, no. 5 (2006): 768-775.
Passeron T et al., “Post-inflammatory hyperpigmentation in acne: Pathogenesis and treatments.” Dermatologic Clinics 32, no. 3 (2014): 291-299.
Bikowski JB et al., “Prevention and management of post-inflammatory hyperpigmentation in acne.” Journal of Drugs in Dermatology 17, no. 9 (2018): 925-932.
Hassim Z et al., “Management of collagen depletion and fat layer loss in acne-prone skin.” Journal of Dermatology 47, no. 5 (2020): 431-437.
Alvarez OM et al., “Botanical extracts for treating acne: Efficacy and safety.” Journal of Cosmetic Dermatology 17, no. 6 (2018): 1067-1074.
Kraft JN et al., “The role of inflammation in acne management.” Journal of Clinical and Aesthetic Dermatology 11, no. 8 (2018): 16-23.
Lim JT et al., “Sun protection and prevention of post-inflammatory hyperpigmentation in acne.” Journal of the American Academy of Dermatology 82, no. 5 (2020): 1236-1245.
Sardana K et al., “Rebound acne and its management: A review.” Indian Journal of Dermatology, Venereology, and Leprology 85, no. 3 (2019): 243-250.
Draelos ZD et al., “Efficacy of natural ingredients in anti-acne treatments.” Journal of Drugs in Dermatology 18, no. 6 (2019): 586-591.
Sadick NS et al., “The impact of collagen production on acne scars.” Journal of Clinical and Aesthetic Dermatology 13, no. 6 (2020): 18-25.
Verallo-Rowell VM et al., “Safety and efficacy of botanical agents in acne management.” Dermatologic Therapy 33, no. 5 (2020): e13963.
Handog EB et al., “Challenges in the management of acne: Prevention and treatment.” Journal of Clinical and Aesthetic Dermatology 9, no. 1 (2016): 15-24.
Narins RS et al., “Long-term complications of injectable soft tissue fillers in acne scars.” Dermatologic Surgery 34, no. 12 (2008): 1574-1579.
Poon TS et al., “Age-related changes in acne and effective management strategies.” Journal of Clinical and Aesthetic Dermatology 14, no. 7 (2021): 32-40.
Nistico SP et al., “Efficacy of botanical formulations for managing acne and hyperpigmentation.” Journal of Dermatological Treatment 31, no. 4 (2020): 395-402.
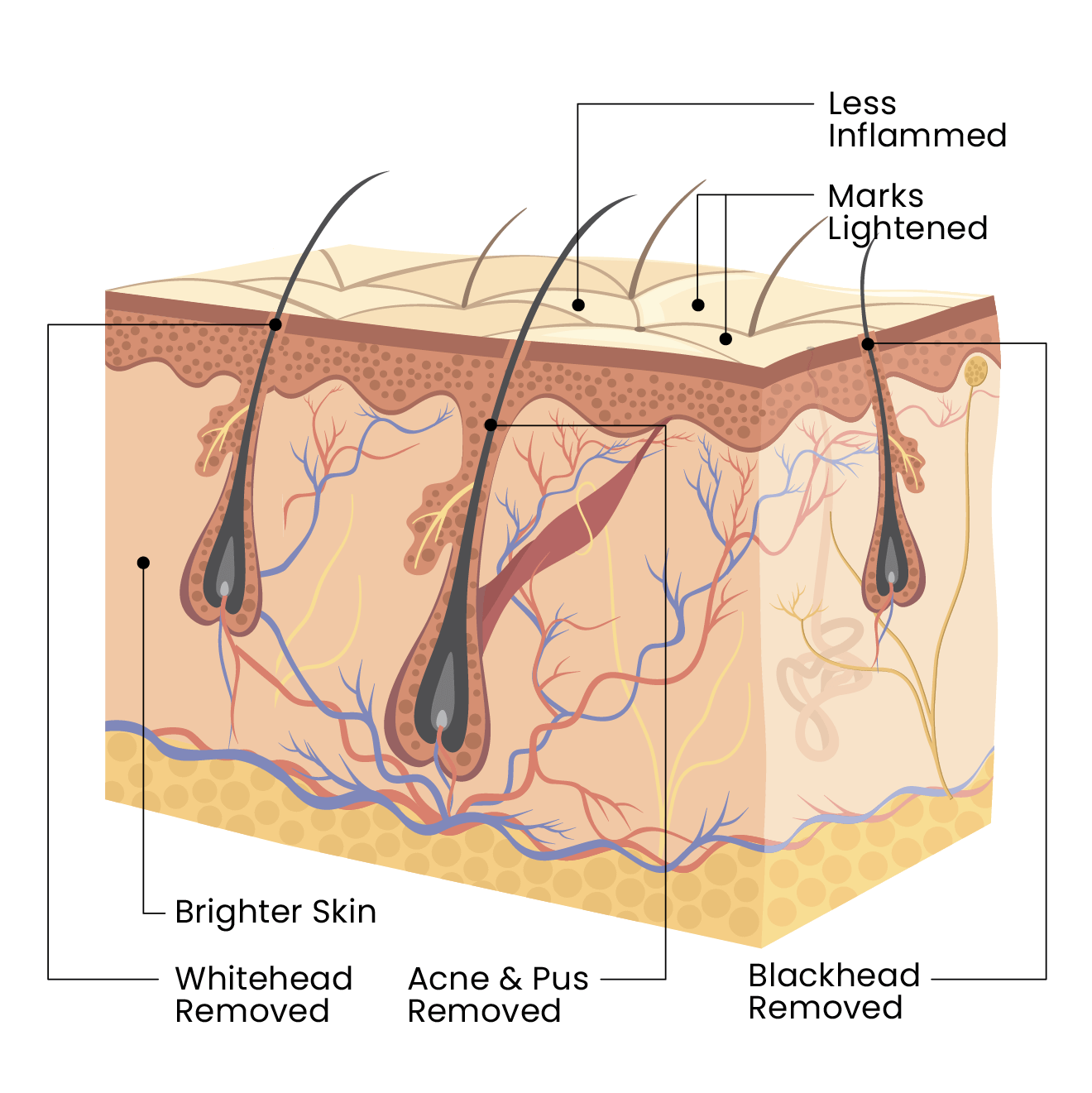
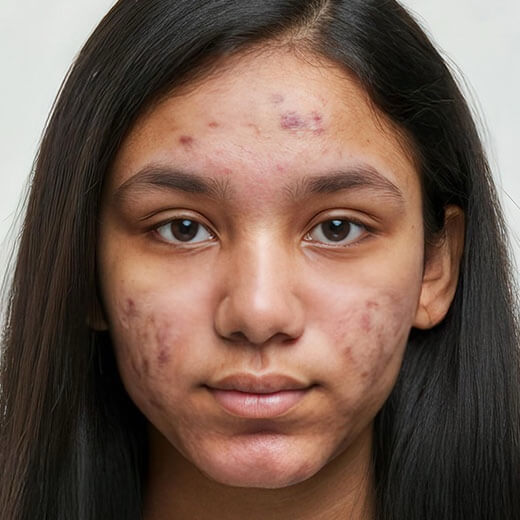
Before & After

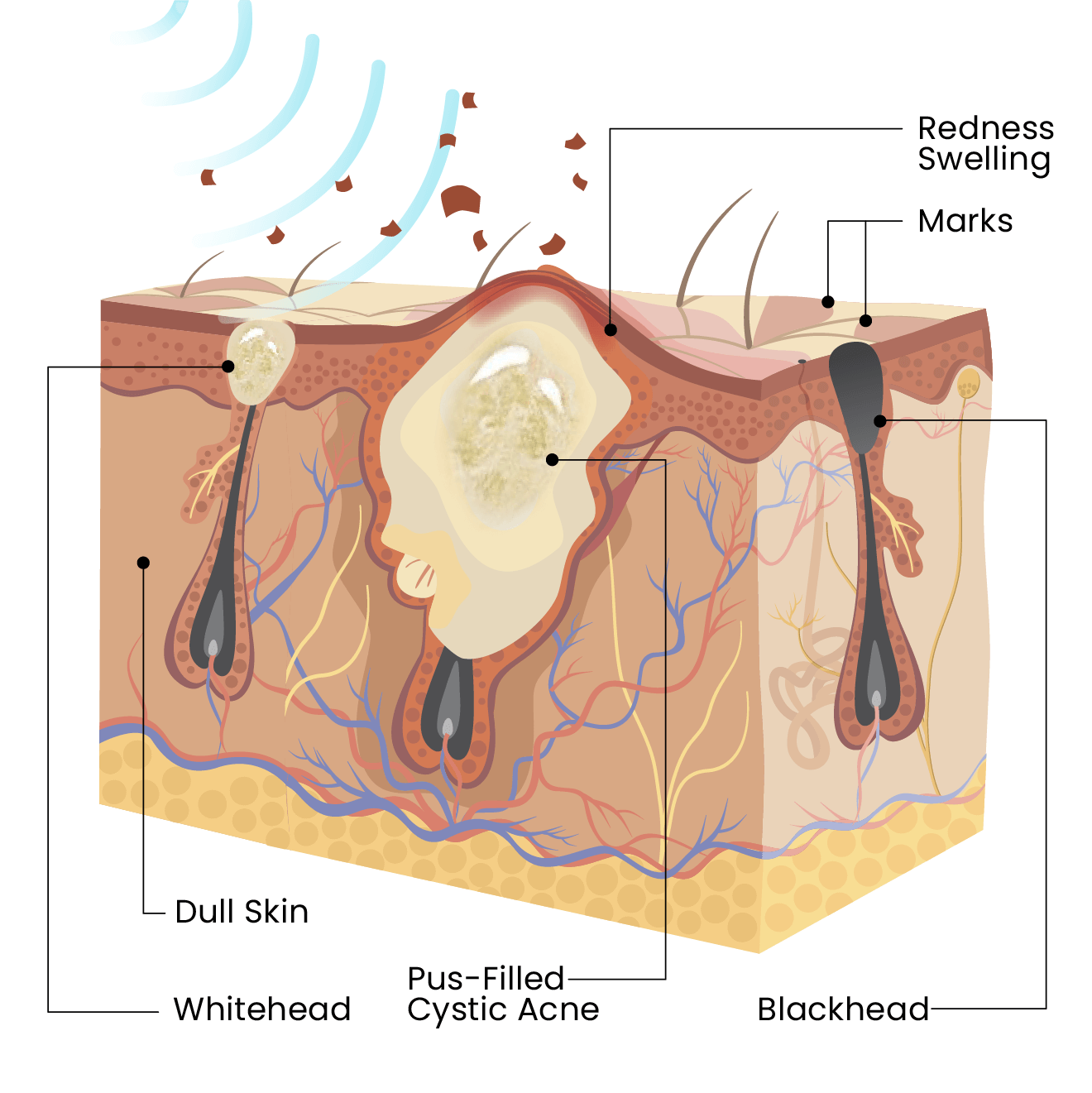
Painful, swollen breakouts triggered by hormonal imbalance, dietary reasons, oral medication, genetics, or skin sensitivity.

Reduced swelling, redness, pus, marks, and blemishes. Skin is calmer, clearer, smoother, and less reactive in 3 sessions.

Breakouts along the chin, jawline, and lower cheeks caused by hormones, stress, skincare and sleep imbalance.

Clearer, healthier, and more balanced skin with fewer flare-ups and visibly reduced hormonal breakouts in 3 sessions.

Brown-red spots and blemishes left after breakouts, caused by picking, melanin response, and UV ray exposure.

Faded dark spots and blemishes. Less blotchiness. Brighter, healthier, more even-toned skin in 3 sessions.
Clogged-enlarged pores, bumps, dull skin caused by environment, sebaceous activity, face masks, skincare.

Smoother, brighter, and clearer skin. Refined texture, reduced congestion, and fewer breakouts in 3 sessions.
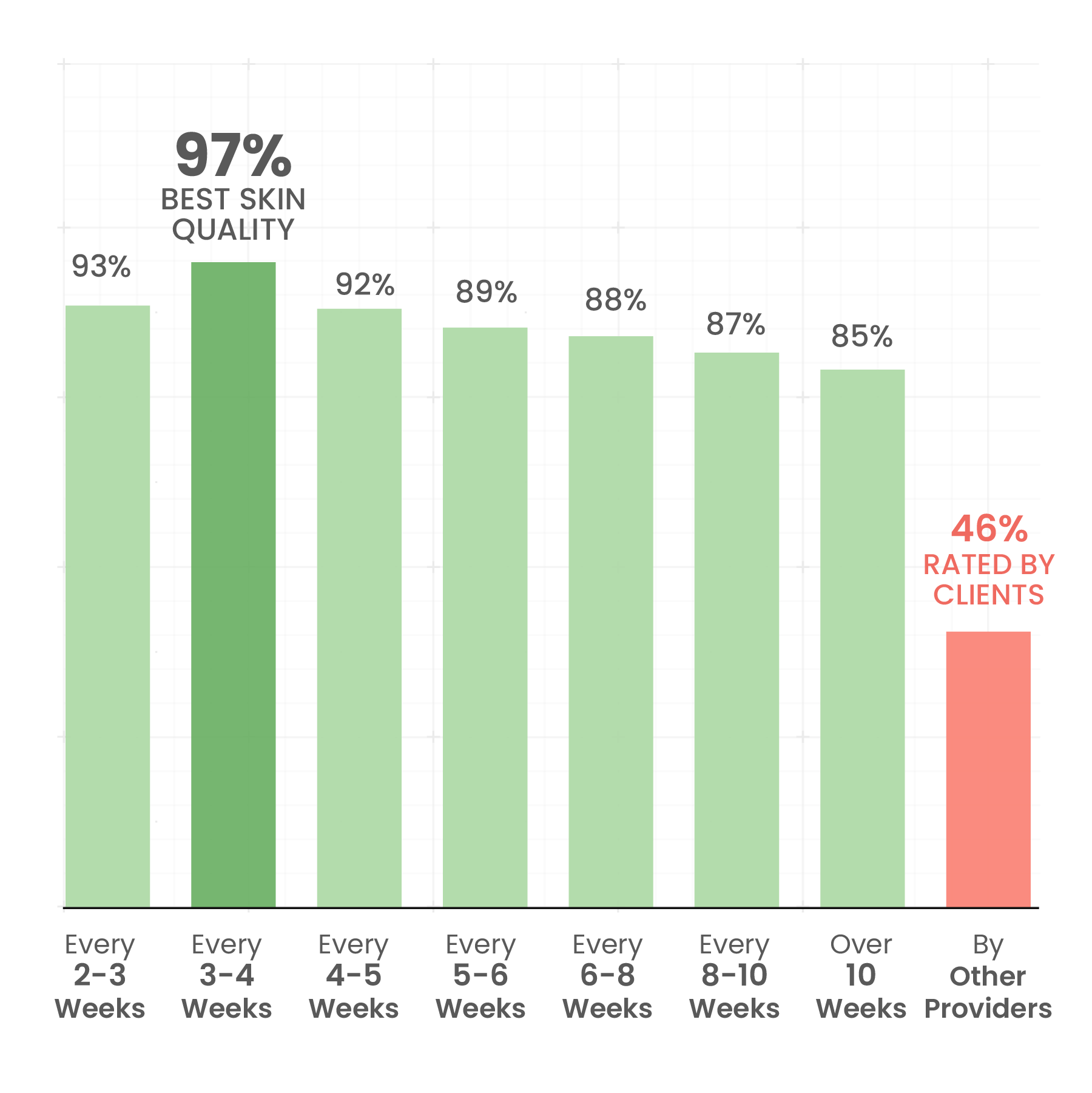
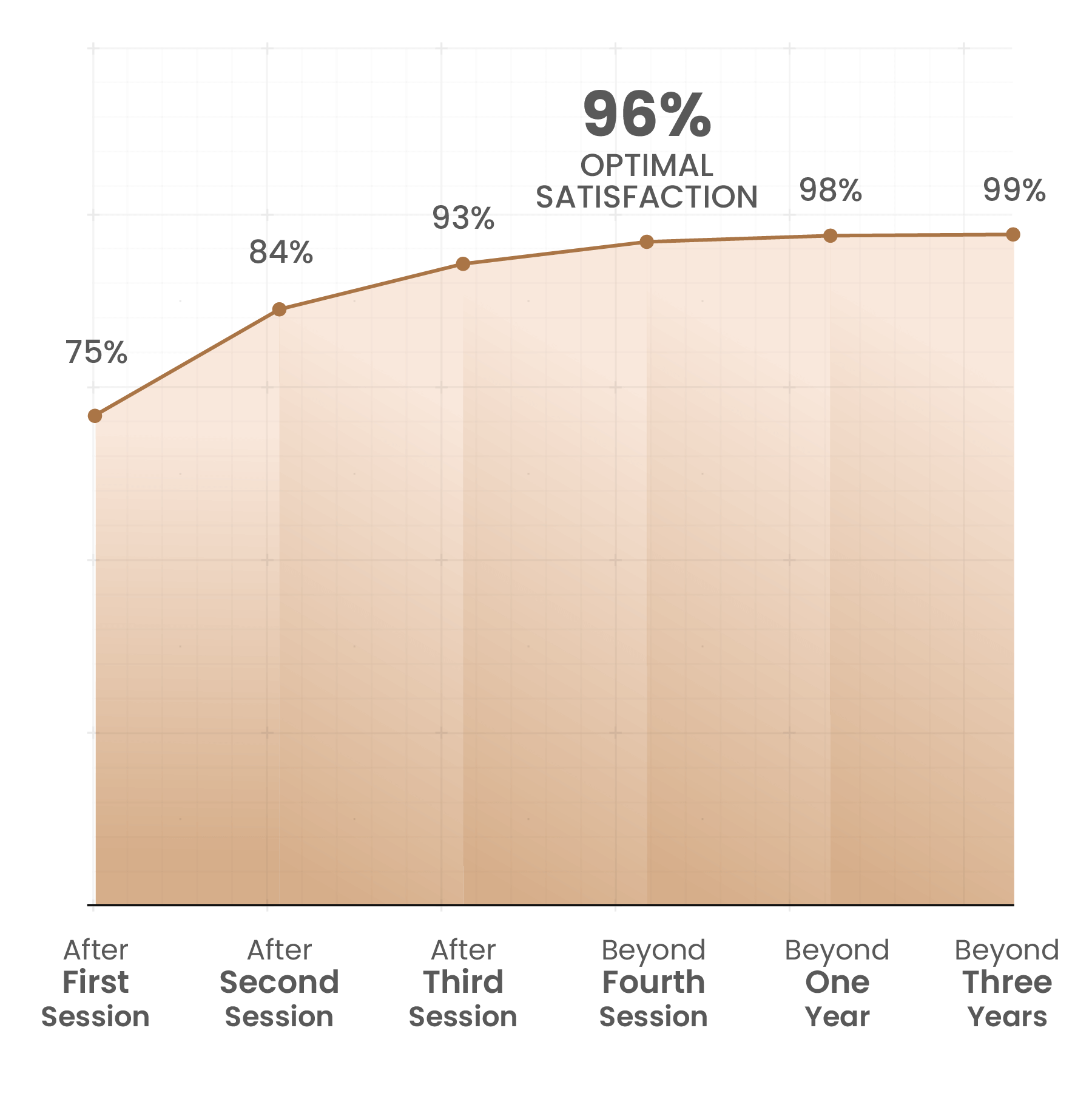
Cumulative Results
What Our Clients Say
Begin Your Clear Skin Reset ✧
What kind of treatments do you offer?
We provide non-invasive, plant-based treatments for acne, pigmentation, aging, hydration, sensitivity, and post-laser or cosmetic care. Visit the Treatments section in our navigation bar to learn more.
Are your treatments suitable for sensitive skin?
Yes, our treatments are gentle and plant-based, making them suitable for sensitive skin. Each session is customised to avoid potential irritants and support your skin’s natural balance.
Can I undergo treatments during pregnancy and postnatal care?
Yes, our treatments are safe throughout pregnancy and postnatal care. They are non-invasive and use plant-based formulas free from retinoids, high-dose salicylic acid, essential oils of concern, and ingredients that may trigger hormonal or systemic responses. We focus on hydration, barrier repair, and calming inflammation, which are key needs during this period.
Please inform us if you are pregnant or breastfeeding so we can tailor your care. You may also consult your doctor for added assurance.
Are your treatments suitable for post-laser recovery?
Yes, we offer treatments to soothe, repair, and strengthen skin after laser or energy-based procedures. For mild cases, a 12-hour gap is sufficient. For more intensive procedures, wait 5 to 10 days.
We recommend PhytoCalm™ or PhytoGlow™ to support recovery. A consultation will help us customise care based on your skin and procedure.
Can I undergo treatments after an aesthetic procedure?
Yes, our treatments support recovery after Botox and fillers by improving skin texture, reducing swelling, and boosting skin health.
PhytoCalm™ and PhytoGlow™ are ideal post-procedure. For more intensive options like PhytoLift™ or PhytoPigment™, wait 3 to 5 days after Botox and 10 to 14 days after fillers. A consultation helps us tailor the safest and most effective care for your skin.
Can I undergo treatments after a cosmetic surgery?
Yes, our treatments can support recovery and enhance skin health after cosmetic surgery. The timing and type of treatment depend on the procedure and your stage of healing.
For minor surgeries like eyelid correction or chin liposuction, we recommend waiting 10 to 14 days until swelling subsides and incisions stabilise. For major procedures such as facelifts or full-face fat grafting, a recovery window of 4 to 6 weeks is advised, or until your surgeon confirms it is safe to proceed.
A consultation will help us customise the safest and most effective plan for your recovery and long-term skin health.
Can children undergo treatments?
Yes, we offer gentle, plant-based treatments suitable for children, especially those dealing with acne, congestion, or sensitive skin. We generally recommend treatments for those aged 10 and above, depending on their skin needs. A consultation will help us assess suitability and customise the safest care plan.
What if I have allergies to certain plants or ingredients?
If you have known allergies, please inform us during your consultation. We will carefully review your history, assess suitability, and customise your treatment and product plan to avoid any potential triggers. Your safety and comfort are always our priority.
Can I undergo treatments if I am on medication?
It depends on your medication and the treatment planned, as some combinations may have contraindications. Most clients on long-term medication experience no issues, but we strongly recommend informing us in advance so we can tailor your care safely. Where needed, you may also consult your doctor to complement our recommendations.
How do I benefit from using your skincare products after treatment?
Using our in-house skincare is strongly recommended to maintain and enhance treatment results. Most clients adopt a personalised regimen designed to support long-term improvement, recovery, and resilience, especially for sensitive or compromised skin.
Each formula is based on real client studies and works in harmony with our treatments without causing fatigue or rebound. Backed by over 20 years of use, they deliver consistent results and peace of mind.
Are your treatments halal-certified?
Our products and treatments are not halal certified. However, we adopt a plant based and conscientious approach to ingredient sourcing, formulation standards, and in clinic practices. We avoid prohibited sources and uphold clean, ethical methods from harvesting and production to professional application, in alignment with sound values and recognised good manufacturing practices.
How often should I receive treatments?
Frequency depends on your skin goals and condition. Most clients benefit from monthly sessions. We will advise a suitable schedule during your consultation. For details on treatment efficacy and timelines, see each treatment page.
What is the average price per treatment?
Prices vary based on the expertise required and the quality, rarity, and potency of our natural ingredients. Most treatments range from S$180 to S$350. We also offer value-added packages for clients seeking consistent or advanced care. For exact pricing, please refer to each treatment’s page.
What forms of payment do you accept?
We accept cash, VISA, and MasterCard, as well as digital payments such as GrabPay and PayLah! For qualifying purchases, we also offer 0% instalment plans via OCBC for 6 or 12 months.
Feel the difference with personalised, non-invasive care.