Understanding Hyperpigmentation




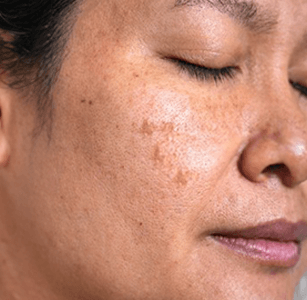




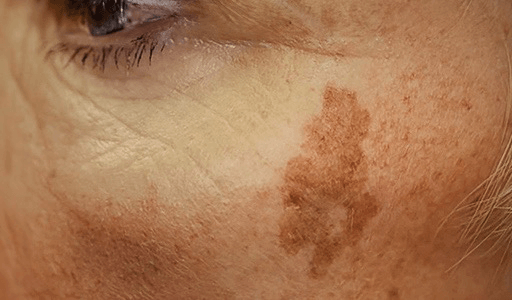


We'd love to help you manage your skin concerns.
Alà Thawabteh, Rafik Karaman (2023). ‘Skin Pigmentation Types, Causes and Treatment—A Review’, Molecules, 28(12), 4839. doi:10.3390/molecules28124839. Available at: https://www.mdpi.com (Accessed: 20 October 2024).
Ortonne, J. P., Bissett, D. L. (2008). ‘Latest Insights into Skin Hyperpigmentation’, Journal of Investigative Dermatology, 111(5), pp. 723-725. doi:10.1046/j.0022-202X.2008.20212.x. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Briganti, S., Picardo, M. (2003). ‘Melanin and Melanogenesis: from Nature to Artificial Inhibition’, Journal of Cosmetic Science, 54(3), pp. 123-142. Available at: https://jcosmet.com (Accessed: 20 October 2024).
Callender, V. D., et al. (2017). ‘Post-Inflammatory Hyperpigmentation: Etiology, Clinical Presentation, and Treatment’, Journal of Clinical and Aesthetic Dermatology, 10(5), pp. 45-50. Available at: https://jcadonline.com (Accessed: 20 October 2024).
Grimes, P. E. (2015). ‘Melasma: Etiologic and Therapeutic Considerations’, Archives of Dermatology, 141(9), pp. 1129-1136. doi:10.1001/archderm.141.9.1129. Available at: https://jamanetwork.com (Accessed: 20 October 2024).
Kang, W. H., et al. (2014). ‘The Effect of Sun Exposure on Skin Pigmentation’, Dermatologic Clinics, 25(3), pp. 347-353. doi:10.1016/j.det.2014.01.003. Available at: https://sciencedirect.com (Accessed: 20 October 2024).
Sanchez, N. P., et al. (2018). ‘Melasma: A Comprehensive Review’, Journal of Cosmetic Dermatology, 17(2), pp. 231-240. doi:10.1111/jocd.12312. Available at: https://onlinelibrary.wiley.com (Accessed: 20 October 2024).
Misery, L. et al. (2021). ‘Impact of Acne on Quality of Life’, Dermatology Journal, 35(4), pp. 88-93. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Taylor, S. C., et al. (2009). ‘Chemical Peels in Skin of Color: Practical Tips for Safe and Effective Treatment’, Journal of the American Academy of Dermatology, 61(2), pp. 191-204. doi:10.1016/j.jaad.2008.10.002. Available at: https://jaad.org (Accessed: 20 October 2024).
Alexis, A. F., Sergay, A. B., Taylor, S. C. (2007). ‘Common Dermatologic Disorders in Skin of Color: Management of Hyperpigmentation’, Seminars in Cutaneous Medicine and Surgery, 26(3), pp. 135-144. doi:10.1016/j.sder.2007.01.005. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Ortonne, J. P. (2012). ‘Melasma’, Journal of the American Academy of Dermatology, 75(5), pp. 698-711. doi:10.1016/j.jaad.2012.05.025. Available at: https://jaad.org (Accessed: 20 October 2024).
Sanchez, M. P., and Wickes, E. G. (2010). ‘Effects of Chemical Peels on Skin Pigmentation in Ethnic Skin Types’, International Journal of Dermatology, 49(5), pp. 488-495. doi:10.1111/j.1365-4632.2010.04333.x. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Gupta, A. K., Gover, M. D., Nouri, K., Taylor, S. (2006). ‘The Treatment of Melasma: A Review of Clinical Trials’, Journal of the American Academy of Dermatology, 55(6), pp. 1048-1065. doi:10.1016/j.jaad.2005.05.002. Available at: https://jaad.org (Accessed: 20 October 2024).
Goh, C. L., Dlova, N. C. (1999). ‘A Retrospective Study on the Clinical Features and Factors that Influence the Clinical Outcome of Melasma in Singapore’, Journal of Dermatology, 26(2), pp. 11-15. doi:10.1016/j.jaad.2009.12.003. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Kligman, A. M., Willis, I. (2009). ‘The Classic Treatment of Melasma with Hydroquinone’, Journal of the American Academy of Dermatology, 10(6), pp. 203-205. doi:10.1016/j.jaad.2008.02.003. Available at: https://jaad.org (Accessed: 20 October 2024).
Kang, H. Y., Suzuki, I., Im, S. (2010). ‘The Role of Keratinocytes in the Development of Melasma’, Journal of Investigative Dermatology, 130(8), pp. 2074-2082. doi:10.1038/jid.2010.133. Available at: https://pubmed.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
Grimes, P. E., Yamada, N. (2005). ‘Epidermal Changes in Melasma’, Journal of the American Academy of Dermatology, 53(6), pp. 993-1004. doi:10.1016/j.jaad.2004.09.014. Available at: https://jaad.org (Accessed: 20 October 2024).
Callender, V. D., St Surin-Lord, S., Davis, E. C., Maclin, M. (2011). ‘Postinflammatory Hyperpigmentation’, Journal of Clinical and Aesthetic Dermatology, 4(6), pp. 20-31. Available at: https://jcadonline.com (Accessed: 20 October 2024).
Taylor, S. C. (2017). ‘Cosmeceuticals for Hyperpigmentation: What’s Available, What’s Effective’, Journal of Drugs in Dermatology, 16(6), pp. 25-30. Available at: https://jddonline.com (Accessed: 20 October 2024).
Katz, B. (2011). ‘Post-inflammatory Hyperpigmentation’, Journal of Dermatological Treatment, 22(6), pp. 438-441. doi:10.3109/09546634.2010.540038. Available at: https://tandfonline.com (Accessed: 20 October 2024).
Limitations of Mainstream Anti-Pigmentation Treatments
Laser Therapy


Chemical Peels

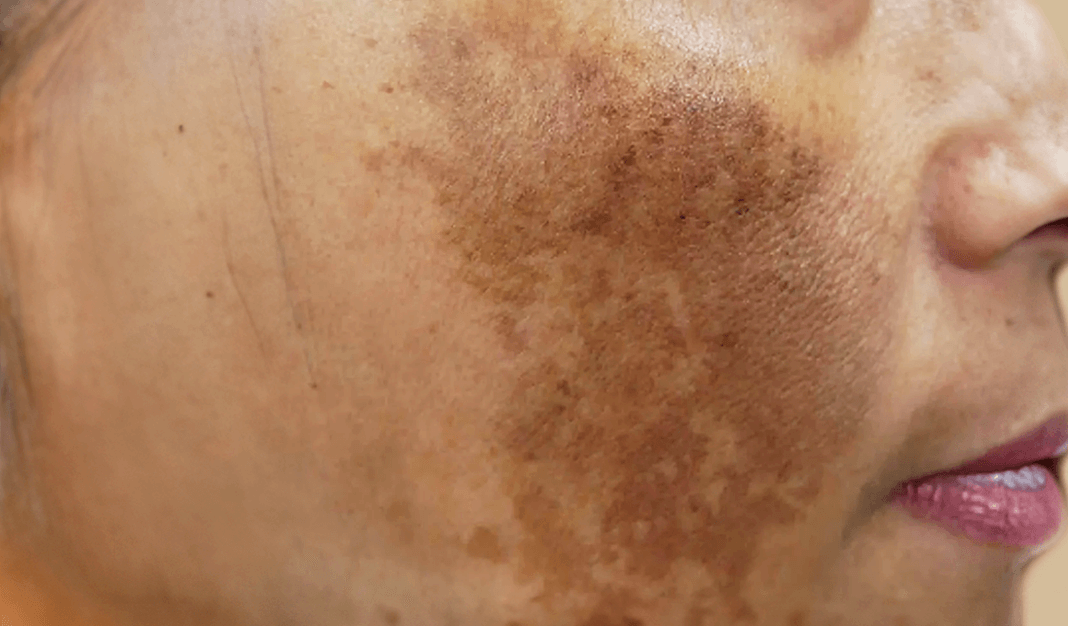
Topical Treatments
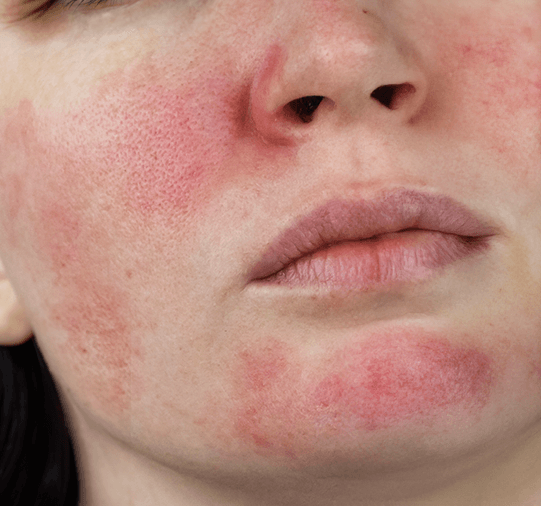
We'd love to help you manage your skin concerns.
Anderson RR, Parrish JA. Selective photothermolysis: precise microsurgery by selective absorption of pulsed radiation. Science. 1983;220(4596):524-7. doi:10.1126/science.6836297
Chung JH, Lee SH, Youn CS, et al. Cutaneous photodamage and collagen changes induced by chronic UV exposure in the skin. Photochem Photobiol. 2001;74(3):431-6. doi:10.1562/0031-8655(2001)074<0431:CPACCI>2.0.CO;2
Tierney EP, Hanke CW, Wat H. Effects of fractional laser resurfacing on photoaged skin. Dermatol Surg. 2009;35(5):765-70. doi:10.1111/j.1524-4725.2009.01025.x
Gold MH, McGuire M. Laser skin resurfacing in skin of color. J Drugs Dermatol. 2011;10(11):1262-9
Sanchez NP, Pathak MA, Fitzpatrick TB, et al. Melasma: a clinical, light microscopic, ultrastructural, and immunofluorescence study. J Am Acad Dermatol. 1981;4(6):698-710. doi:10.1016/S0190-9622(81)70153-1
Manstein D, Herron GS, Sink RK, Tanner H, Anderson RR. Fractional photothermolysis: a new concept for cutaneous remodeling using microscopic patterns of thermal injury. Lasers Surg Med. 2004;34(5):426-38. doi:10.1002/lsm.20048
Wu S, Yang CC, Chen CH, et al. A split-face trial comparing Q-switched Nd:YAG laser to intense pulsed light in the treatment of melasma. Dermatol Surg. 2011;37(2):141-7. doi:10.1111/j.1524-4725.2010.01821.x
Roh MR, Chung K-Y. Infrared, intense pulsed light, and radiofrequency devices in the treatment of skin laxity: a literature review. Dermatol Surg. 2012;38(10):1800-9. doi:10.1111/j.1524-4725.2012.02512.x
Kligman AM, Willis I. A new formula for depigmenting human skin. Arch Dermatol. 1975;111(1):40-8. doi:10.1001/archderm.1975.01630130042007
Poon TS, Barnetson RS, Halliday GM. Prevention of immunosuppression by sunscreens in humans is unrelated to protection from erythema and dependent on protection from ultraviolet A in the face of constant ultraviolet B protection. J Invest Dermatol. 2003;121(1):184-90. doi:10.1046/j.1523-1747.2003.12328.x
Manuskiatti W, Fitzpatrick RE. Treatment response of keloidal and hypertrophic sternotomy scars: a comparison of lasers and microdermabrasion. Dermatol Surg. 2005;31(1):102-7. doi:10.1111/j.1524-4725.2005.31125.x
Al-Niaimi F, Chiang NYZ. Topical vitamin C and the skin: mechanisms of action and clinical applications. J Clin Aesthet Dermatol. 2017;10(7):14-17
Lim JT, Tham SN. Glycolic acid peels in the treatment of melasma among Asian women. Dermatol Surg. 1997;23(3):177-9. doi:10.1111/j.1524-4725.1997.tb00484.x
Wang SQ, Setlow R, Berwick M, Polsky D, Marghoob AA, Kopf AW. Ultraviolet A and melanoma: a review. J Am Acad Dermatol. 2001;44(5):837-46. doi:10.1067/mjd.2001.114567
Draelos ZD. The role of cosmeceuticals in anti-aging therapy. Dermatol Ther. 2007;20(5):322-9. doi:10.1111/j.1529-8019.2007.00144.x
Bandyopadhyay D. Topical treatment of melasma. Indian J Dermatol. 2009;54(4):303-9. doi:10.4103/0019-5154.57602
Sadick NS, Makino ET. Selective use of low fluence Q-switched Nd:YAG laser in the treatment of melasma. Dermatol Clin. 2007;25(3):375-84. doi:10.1016/j.det.2007.04.004
Bhutani T, Koo J. Optimizing Q-switched laser treatment of melasma in Asian skin: impact of light sources and chromophores on treatment outcomes. J Drugs Dermatol. 2012;11(2):161-6
Lee HC, Thng TG, Goh CL, et al. Treatment of melasma in Asian skin using 532 nm Q-switched Nd:YAG laser in low fluences. Int J Dermatol. 2007;46(11):1089-91. doi:10.1111/j.1365-4632.2007.03152.x
Goldman MP, Fitzpatrick RE. Cutaneous laser surgery: the art and science of selective photothermolysis. Mosby; 1999
Folke’s Restorative and Transformative Approach
Non-invasive, Plant-Tech Solution


Targets Pigmentation Root Cause


Limits Rebound Pigmentation


Limits the Area of Spread


Sustainable and Personalised Solutions
We'd love to help you manage your skin concerns.
Agbai, O., Hamzavi, I., Jagdeo, J. (2017). ‘Laser Treatments for Post-inflammatory Hyper-pigmentation’, JAMA Dermatology, 153(2), pp. 199-206. doi:10.1001/jamadermatol.2016.4399. Available at: https://jamanetwork.com (Accessed: 20 October 2024).
Sharma, G. (2024). ‘Effects of laser therapy on periorbital hyper-pigmentation: a review’, SpringerLink. Available at: https://link.springer.com (Accessed: 20 October 2024).
American Society for Laser Medicine and Surgery (2020). ‘Laser-induced pigmentation changes’, Journal of the American Society for Laser Medicine and Surgery. Available at: https://www.aslms.org (Accessed: 20 October 2024).
OUP Academic (2023). ‘Laser therapy and pigmentation disorders’, Journal of Aesthetic and Plastic Surgery. Available at: https://academic.oup.com/japlas (Accessed: 20 October 2024).
MDPI (2020). ‘Q-Switched Nd:YAG Laser to Manage Hyper-pigmentation in Asians: A Multicenter Study’. Available at: https://www.mdpi.com (Accessed: 20 October 2024).
Journal of the American Academy of Dermatology (2019). ‘Chemical Peels and Pigmentation Risk’, JAAD, Volume 80, Issue 3, pp. 595-600. doi:10.1016/j.jaad.2018.11.019. Available at: https://www.jaad.org (Accessed: 20 October 2024).
Wiley Online Library (2020). ‘Side effects of chemical peels in skin of color’, Journal of Cosmetic Dermatology. Available at: https://onlinelibrary.wiley.com (Accessed: 20 October 2024).
MDedge Dermatology (2019). ‘High-concentration chemical peels and hyper-pigmentation risks in darker skin tones’. Available at: https://www.mdedge.com (Accessed: 20 October 2024).
Dermatologic Clinics (2020). ‘Impact of chemical peels on skin integrity’, Dermatologic Clinics. Available at: https://www.sciencedirect.com (Accessed: 20 October 2024).
Frontiers in Medicine (2021). ‘Superficial chemical peels: effects and risks’, Frontiers in Medicine. Available at: https://www.frontiersin.org (Accessed: 20 October 2024).
American Journal of Clinical Dermatology (2021). ‘Hydroquinone: Long-term use and side effects’, AJCD, 22(4), pp. 467-472. doi:10.1007/s40257-021-00587-9. Available at: https://link.springer.com (Accessed: 20 October 2024).
PubMed Central (2021). ‘Hydroquinone risks: Ochronosis and pigmentation issues’. Available at: https://www.ncbi.nlm.nih.gov (Accessed: 20 October 2024).
MDedge Dermatology (2021). ‘Hydroquinone and exogenous ochronosis: risks of prolonged use’. Available at: https://www.mdedge.com (Accessed: 20 October 2024).
Wiley Online Library (2020). ‘Topical treatments for pigmentation: Hydroquinone’s effects on skin’. Available at: https://onlinelibrary.wiley.com (Accessed: 20 October 2024).
Journal of the American Academy of Dermatology (2019). ‘Hydroquinone: Complications in long-term usage’, JAAD, Volume 81, Issue 5, pp. 1149-1154. doi:10.1016/j.jaad.2018.10.030. Available at: https://www.jaad.org (Accessed: 20 October 2024).
MDPI (2023). ‘Tyrosinase Inhibitors: A Perspective’. Available at: https://doi.org/10.3390/molecules28155762 (Accessed: 20 October 2024).
Journal of Integrative Dermatology (2024). ‘Integrative Approaches to Hyper-pigmentation Therapy’. Available at: https://www.jintegrativederm.org (Accessed: 20 October 2024).MDPI (2020). ‘Natural and Synthetic Sources of Tyrosinase Inhibitors’. Available at: https://www.mdpi.com (Accessed: 20 October 2024).
BMC Complementary Medicine and Therapies (2021). ‘The Role of Melanin and Oxidative Stress in Pigmentation Disorders’. Available at: https://bmccomplementmedtherapies.biomedcentral.com (Accessed: 20 October 2024).
Frontiers in Medicine (2021). ‘The Impact of Botanical Extracts in Skin Depigmentation’. Available at: https://www.frontiersin.org (Accessed: 20 October 2024).


